Executive Summary:
Chronic pain affects millions of people worldwide. It affects both quality of life and healthcare systems. Historically, opioid-based treatment has been used for pain management, but its short duration of action and high rates of risk—including addiction, dependence, and overdose—have prompted a move toward safer and longer-acting alternatives. Neuromodulation, with appropriate methods, can be a good non-pharmacological treatment. It includes spinal cord stimulation (SCS), transcranial magnetic stimulation (TMS), and peripheral nerve stimulation (PNS). These treatments are typically custom-made, minimally invasive, and even reversible, thereby providing relief with minimal side effects. Neuropathic pain, failed back surgery syndrome, and complex regional pain syndrome are some of the conditions that are treated with neuromodulation. As neuromodulation technologies evolve further with AI and closed-loop systems, the treatment of chronic pain is being disrupted with an emphasis on long-term relief, safety, and quality of life.
1. Introduction:
Chronic pain is like an alarm that keeps ringing for several months or even years. Sometimes it’s there all the time; other times it comes and goes. It can strike anywhere in our body and come from countless causes. Pain is a primary reason people seek medical care. When pain lasts for long durations, it does not just affect the body but also impacts physical, mental, and emotional health [1] [2]. Chronic pain is a very difficult problem affecting millions of people throughout the world. It poses enormous challenges for individuals, families, as well as for healthcare delivery.
Over the centuries, opioids have been used to treat moderate to severe pain because of their strong analgesic effect. However, opioids can also cause serious side effects such as overdosing, addiction, tolerance, dependence, stomach bleeding, kidney problems, and heart issues. Because of these risks, there is a need for safer and more effective ways to treat chronic pain without adverse effects. In recent years, patient care has moved away from mainly using medications towards behavioural and procedural treatments like neuromodulation. Neuromodulation is a growing field in pain medicine that uses various electrical therapies (non-invasive, minimally invasive, and surgical) to manage chronic pain safely, without damaging body tissues or causing major side effects [5], [6].
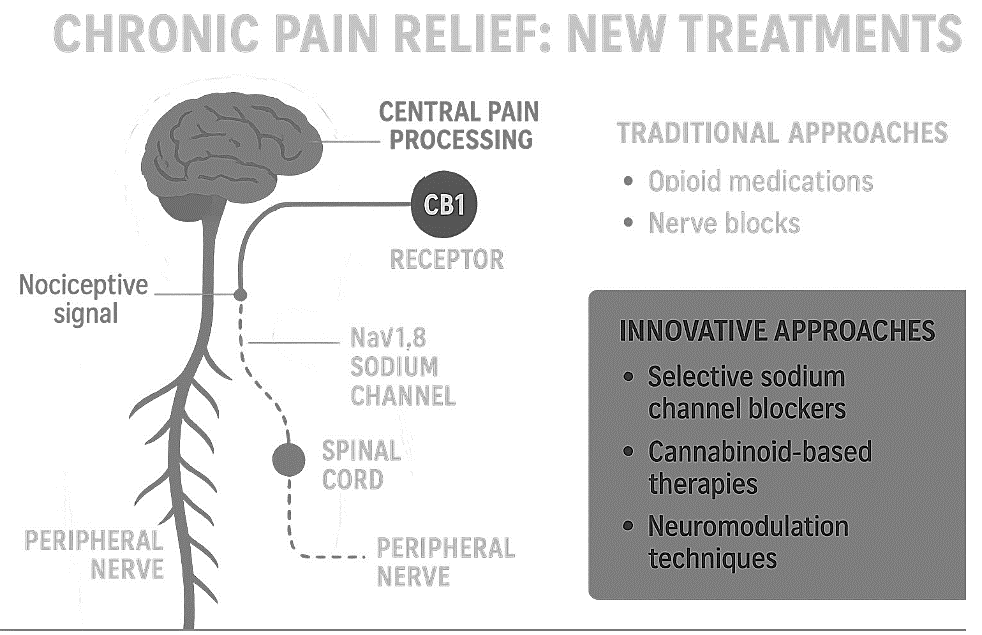
2. Chronic pain relief new treatment vs. traditional opioid treatment
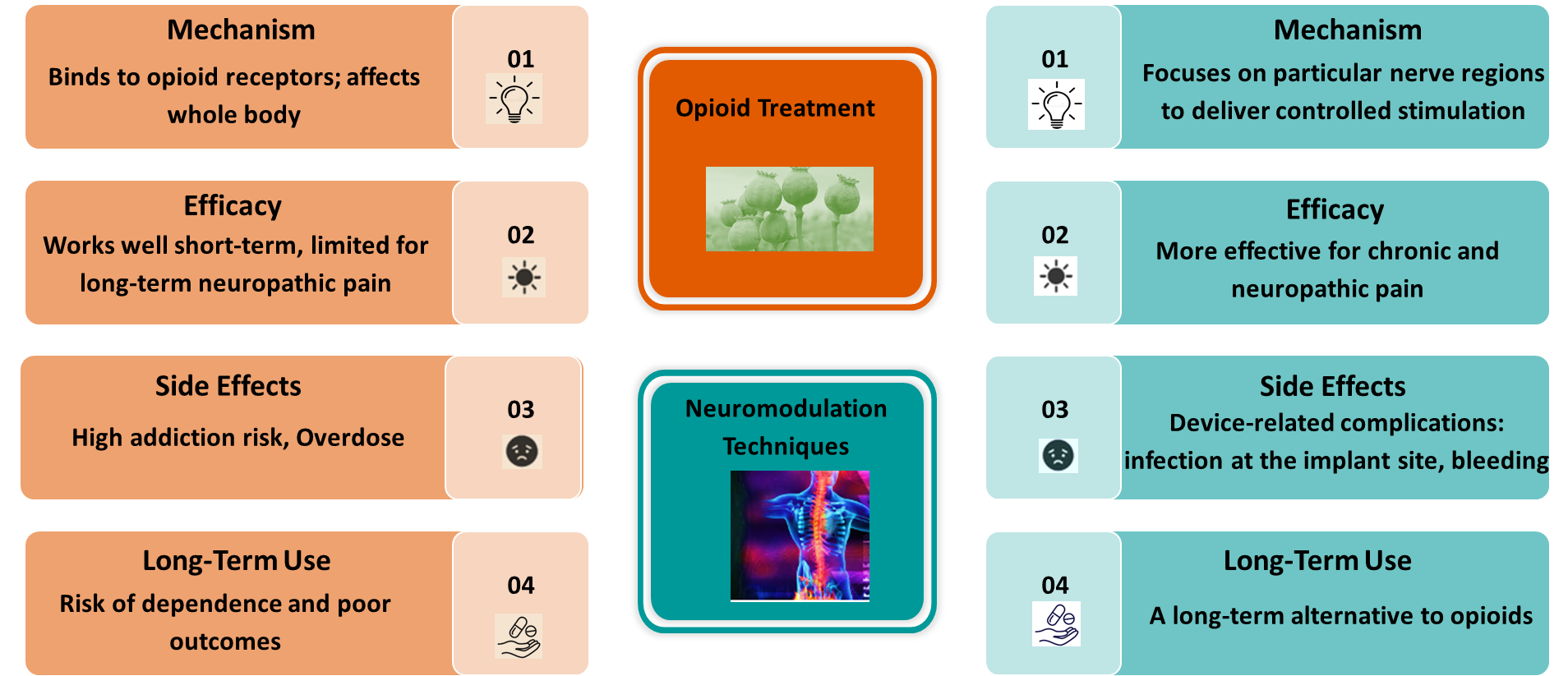
3. Opioids in Pain Management: A Traditional Approach’s Rise and Decline
For millennia, opioids have been considered the most powerful drugs for the treatment of pain. Their analgesic properties make them a good option for managing severe and chronic pain. The term "opioids" refers to compounds that bind with opiate receptors. Opioids are a broad class of drugs that include natural derivatives of the opium poppy, as well as synthetic and semi-synthetic agents designed to copy their pain-relieving effects. Opioids show their effect by binding to specific receptors known as opioid receptors, located in the central nervous system (such as the brain and spinal cord) and some peripheral parts of the body. They modulate pain in both the central and peripheral nervous systems. There are three types of receptors: mu (μ), delta (δ), and kappa (κ). After receptor activation, they cause physiological effects such as analgesia, euphoria, respiratory depression, and sedation [9] [10].
- Most clinically applied opioids have the mu receptors as their main targets, whose activation is linked to pain alleviation, euphoria, respiratory depression, and physical dependence.
- Delta receptors, less well documented, are thought to contribute to mood control and analgesia.
- Kappa receptors, upon stimulation, may cause analgesia along with dysphoria and hallucinations.
Recent studies show that opioid receptors work in more complicated ways than we used to believe. Some drugs can target only specific parts of these receptors, a concept called "biased agonism."
3.1 Crisis:
Their role in the long-term treatment of chronic non-cancer pain is, however, controversial for many reasons. The opioid crisis started in the late 1990s when some pharmaceutical companies claimed that patients would not become addicted to opioid pain relievers. This assurance resulted in a rise in opioid prescriptions, which led to extensive misuse. Later, the highly addictive nature of opioids was recognized, which became a major contributor to the crisis. Currently, the opioid crisis continues to be deeply troubling. Over 100,000 overdose fatalities occurred in the U.S. in 2021 alone, and synthetic opioids like fentanyl are the leading cause. Even though prescription rates have decreased since 2012, opioid abuse persists. The use of fentanyl and other synthetic opioids has worsened the crisis, as these heighten the risk of overdose. The overdoses have caused multiple deaths. With decreased prescription rates, opioid-related deaths continue to increase, highlighting the need for innovative approaches apart from medications [3] [7]. The opioid epidemic has strained healthcare systems and contributed to significant mortality.
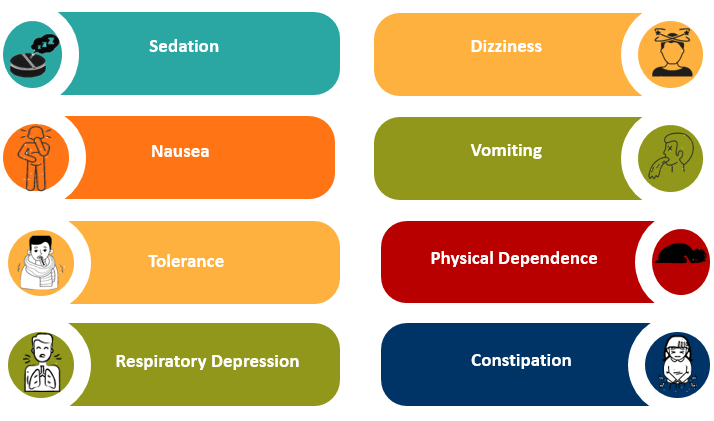
3.2 Side effects:
Common side effects of opioid administration include [11].
4. Neuromodulation: A Paradigm Shift
Neuromodulation is a treatment that uses electric and magnetic stimuli to change nervous system activity and alter how pain feels to the body or brain. Neuromodulation affects several neural pathways that carry pain signals, blocking or changing those signals, which can provide better and longer-lasting relief than conventional treatments [12]. It can involve various invasive and non-invasive techniques, which can be classified based on how they work [13].
4.1 Neuromodulation Mechanisms of Action
The human nervous system has the ability to change its structure and function in response to different stimuli. This ability is known as neuroplasticity. Different types of neuromodulation work in their own ways (figure 1), but they all aim to support neuroplasticity [13]. Both the way nerve cells respond to signals (such as alterations in ion channels that impact cell activity) and how they communicate (known as synaptic plasticity) may change as a result of neuromodulation [13].
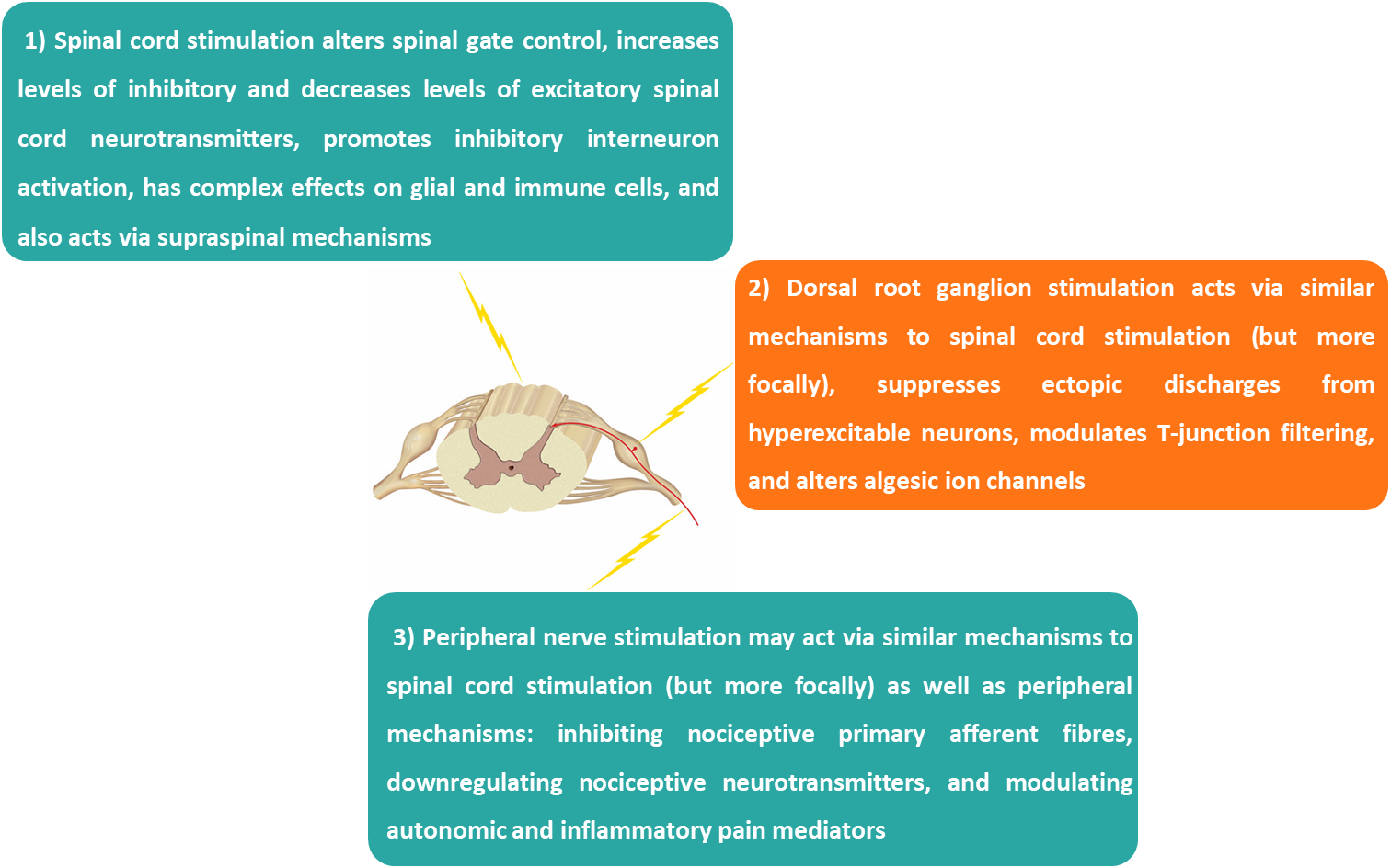
Various levels of change can result from stimulation:
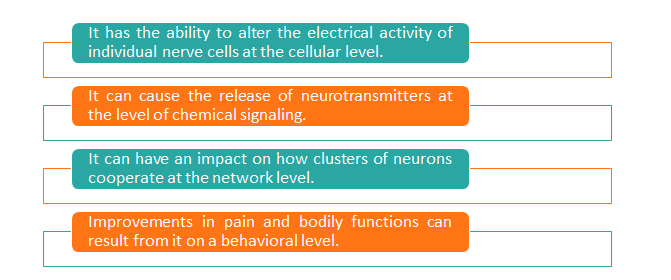
Even brief neuromodulation can result in long-lasting alterations to both neuronal and non-neuronal activity, even after the stimulation has ended. The use of neuromodulation earlier in treatment is becoming more popular, possibly even prior to the onset of severe symptoms. This concept is being discussed more at conferences and is a component of recent studies. Over time, neuromodulation may lose its effectiveness for a number of reasons. Predicting who will benefit from neuromodulation is a challenge, though. A person's age, sex, mental health, genetics, the type of stimulation they receive, the reason for their pain, and the timing of treatment are just a few of the variables that can affect the results [13].
Neuromodulation's effects can diminish with time, just like those of many other analgesic treatments. A well-known study by Kemler and colleagues showed that people with complex regional pain syndrome (CRPS) benefited from spinal cord stimulation (SCS), but the benefits dissipated after only two years.
Reasons for diminished effectiveness can include:
- Maladaptive neuroplasticity: the possibility that the nervous system will become too used to the repeated stimulation.
- The illness may worsen further.
- The placebo effect might not last long.
- Lead migration and other complications.
Lead migration and other complications will likely become less common as technology continues to miniaturize and become more advanced.
4.2 Different forms of neuromodulation:
Neuromodulation involves both invasive and non-invasive methods that are grouped according to the type of stimulation used. These several forms of neuromodulation techniques expand the applicability of neuromodulation across diverse pain conditions. One of the most commonly used in neuropathic pain treatment is spinal cord stimulation (SCS) [13] [22].
4.2.1 Invasive Methods:
Invasive neuromodulation involves a surgical implant, usually at the brain or spinal cord. As part of the surgery, electrodes are implanted for electrical stimulation to modulate neural signals related to pain, thus changing the way pain stimuli are processed and reacted to by the nervous system. Different types of invasive methods are: [23]
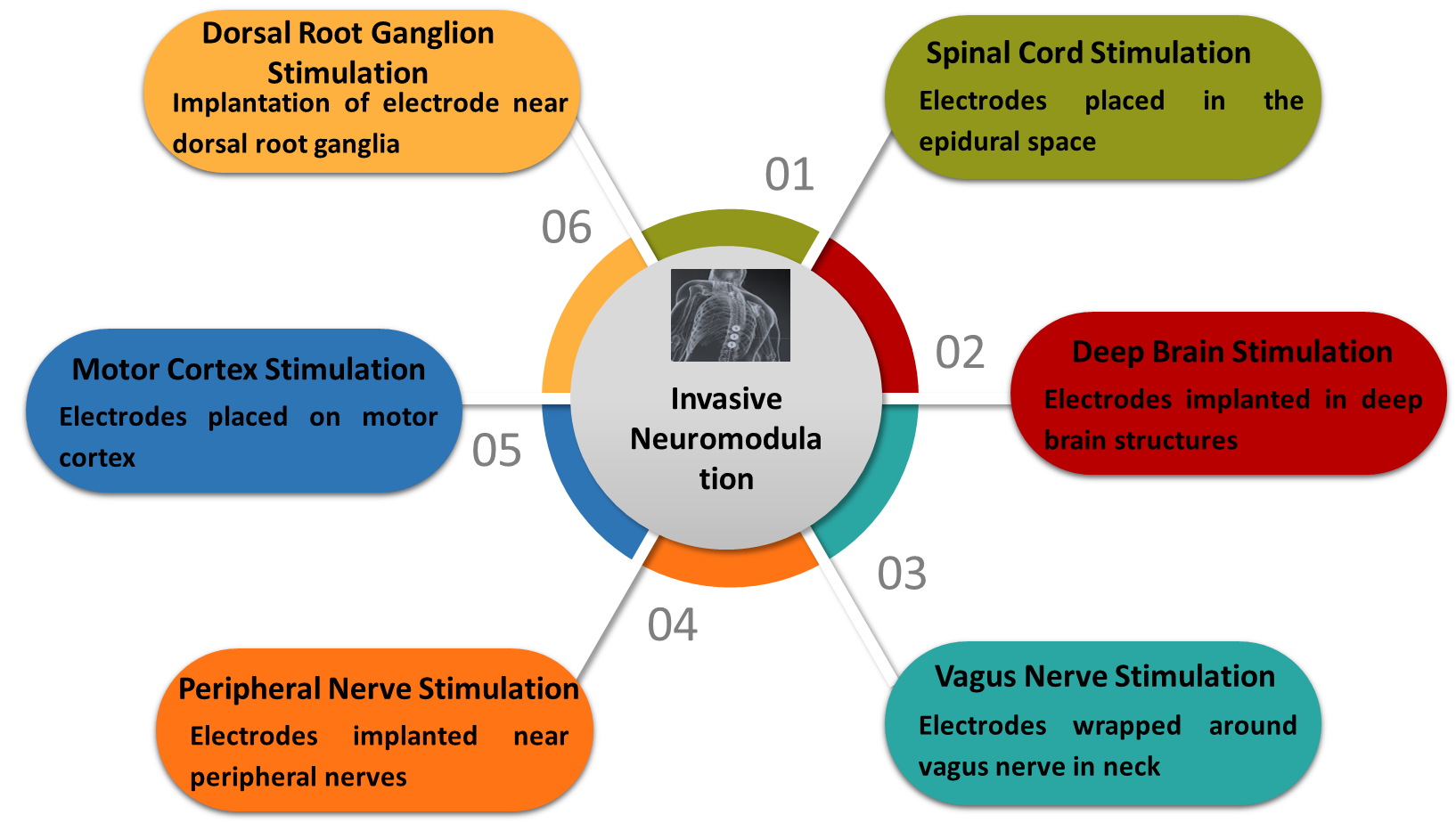
4.2.2 Non-Invasive Methods:
Non-invasive neuromodulatory methods do not need surgery or a trial period, which makes them suitable for earlier use in patient care and often fits well into a team-based treatment model. There are a few drawbacks, however, for these techniques. They are usually administered in the form of multiple sessions, and there is great heterogeneity in stimulation protocols in studies and in clinical practice. The requirement for multiple treatments points to an area which needs further systematic study in order to maximize treatment regimens and find patterns of patient response. Different types of non-invasive methods are: [13]
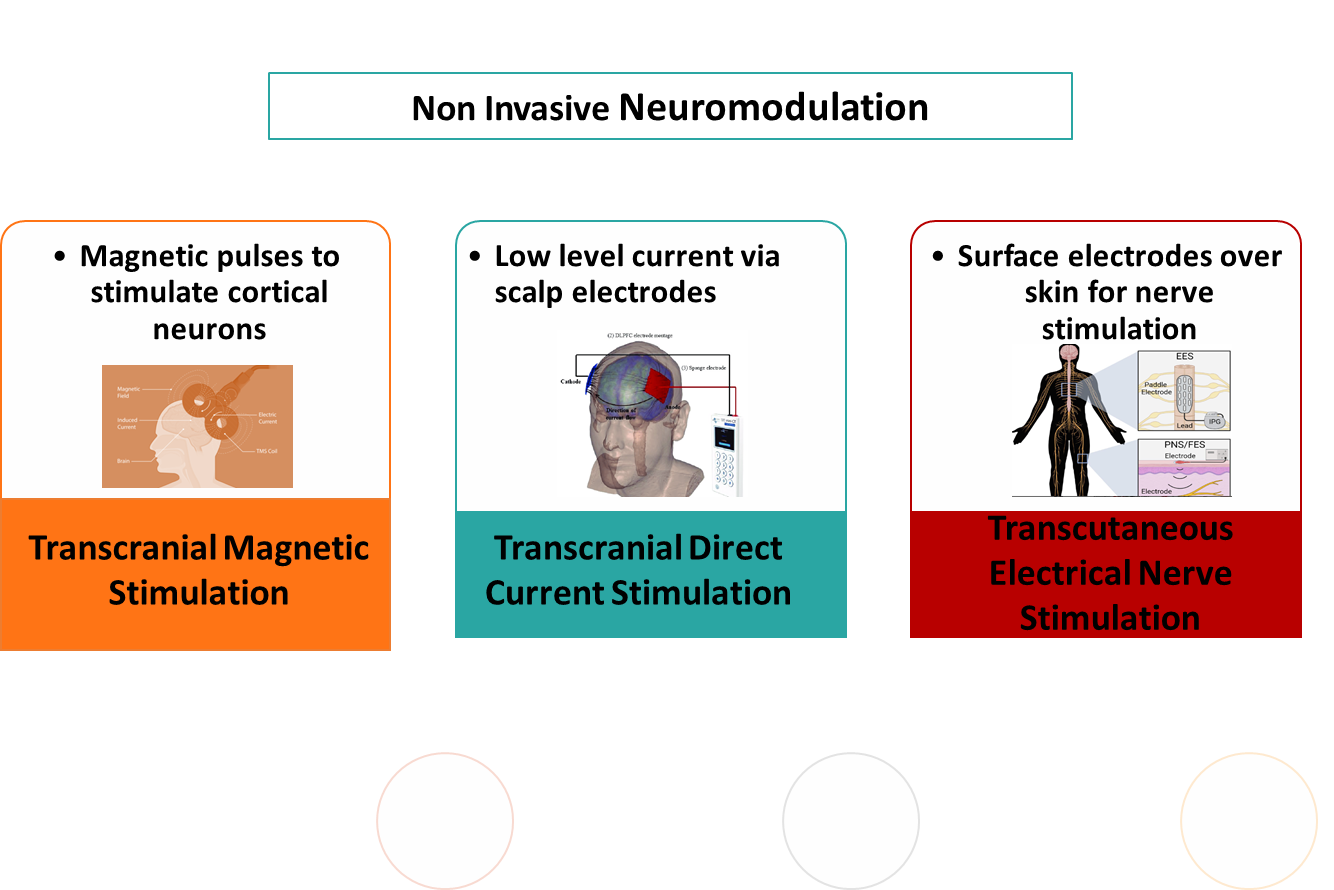
4.2.3 Comparison of neuromodulation techniques.
| Technique | Mechanism | Clinical Application | Advantages |
|---|---|---|---|
| Spinal cord stimulation (SCS) | Inhibits nociceptive transmission | Chronic neuropathic pain | Long-term pain relief |
| Deep brain stimulation (DBS) | Modulates deep brain pain pathways | Refractory pain conditions | Effective for movement disorders & pain |
| Transcranial magnetic stimulation (TMS) | Alters cortical excitability | Chronic pain & mood disorders | Non-invasive |
| Transcranial direct current stimulation (tDCS) | Modifies neuronal activity | Pain modulation & rehabilitation | Low cost & portable |
| Peripheral Nerve Stimulation (PNS) | Electrical impulses applied to peripheral nerves to modulate pain signals. | Chronic post-surgical pain, Neuropathic pain, Migraines, CRPS, Phantom limb pain |
|
| Vagus Nerve Stimulation (VNS) | Stimulates the vagus nerve using an implanted device | Epilepsy, treatment-resistant depression, cluster headaches | Long-term therapy |
| Dorsal Root Ganglion Stimulation (DRG) | Electrical stimulation of the dorsal root ganglion modulates sensory neuron activity, disrupting abnormal pain signal transmission to the CNS. | Complex Regional Pain Syndrome (CRPS), Focal neuropathic pain |
|
| Motor Cortex Stimulation | Epidural electrodes placed over the motor cortex modulate thalamocortical and corticospinal pathways involved in pain processing. | Central (neuropathic) pain, Post-stroke pain | Useful for central pain syndromes |
| Transcutaneous Electrical Nerve Stimulation (TENS) | Low-voltage electrical stimulation applied to the skin activates large-diameter afferent fibers, inhibiting pain signals via the gate control theory. | Osteoarthritis, Postoperative pain, Low back pain |
|
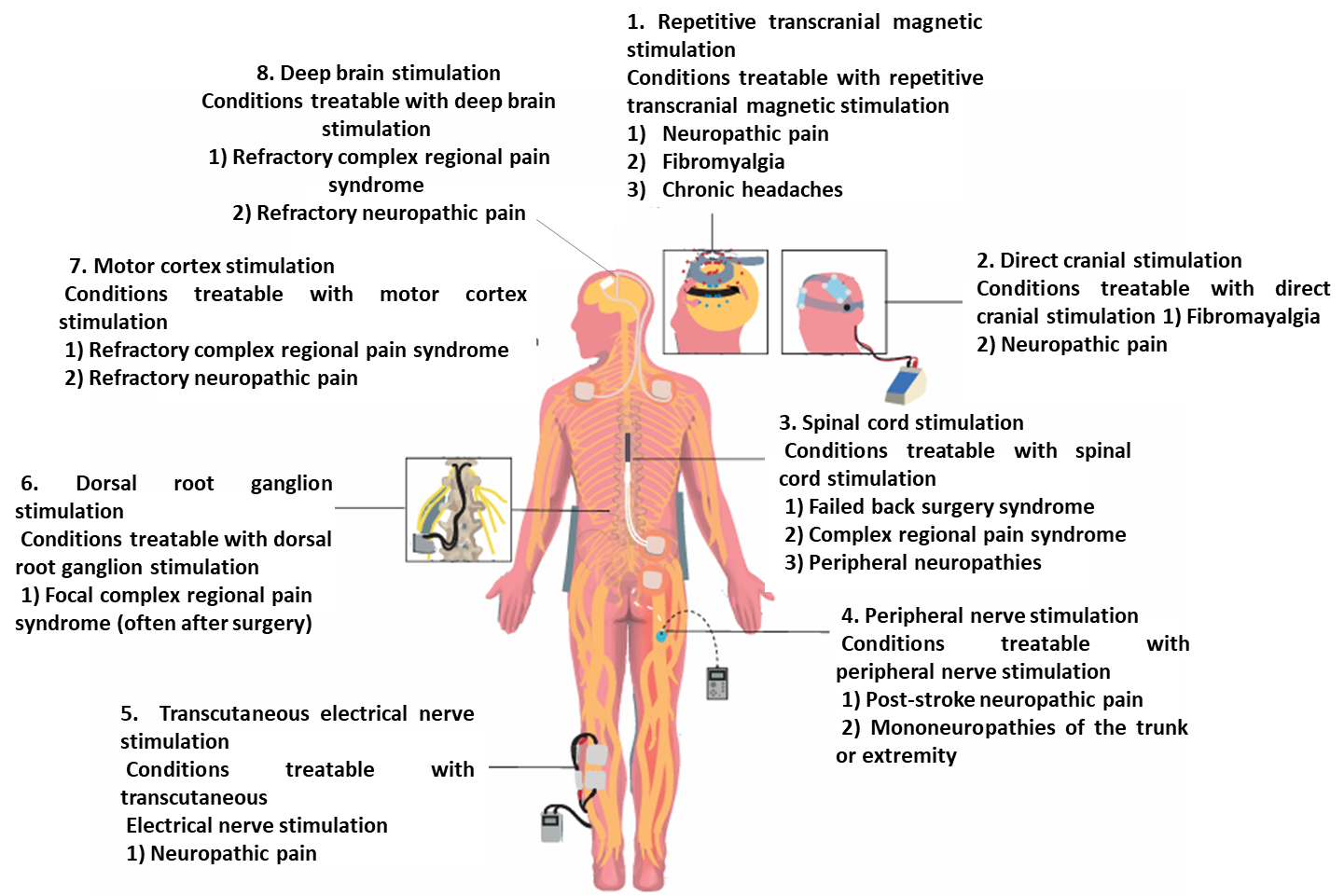
Figure 2: Different forms of neuromodulation and the conditions most amenable to treatment
4.3 Spinal Cord Stimulation
For many years, SCS has been one of the most effective treatments for chronic pain, being minimally invasive and non-opioid. A small device called a spinal cord stimulator is implanted near the spinal cord. Through tiny wires (electrodes) positioned close to the spinal cord, more precisely in the epidural space directly behind the dorsal columns, this device transmits mild electrical signals to specific areas of the spine. Prior to pain signals reaching the brain, these signals assist in blocking them. Patients typically experience a tingling sensation, known as paresthesia, which replaces the perception of pain [13] [14] [17].
4.3.1 How Does SCS Work?
Although research on how exactly SCS reduces pain is ongoing, it is known to work by:
- Activating the large sensory nerve fibers (A-beta fibers), which prevent smaller, chronic pain-specific fibers (C-fibers and A-delta fibers) from sending pain signals.
- Calming down overexcited neurons in the spinal cord’s dorsal horn, which helps tone down the system's sensitivity to pain.
- Stopping the overactivation of glial cells, which reduces inflammation—a big player in chronic pain.
- Influencing regions like the thalamus, frontal cortex, and limbic system that are involved in the perception of emotional and sensory pain by activating higher brain pathways (supraspinal mechanisms) [14].
4.3.2 Why SCS Is Better Than Other Therapies?
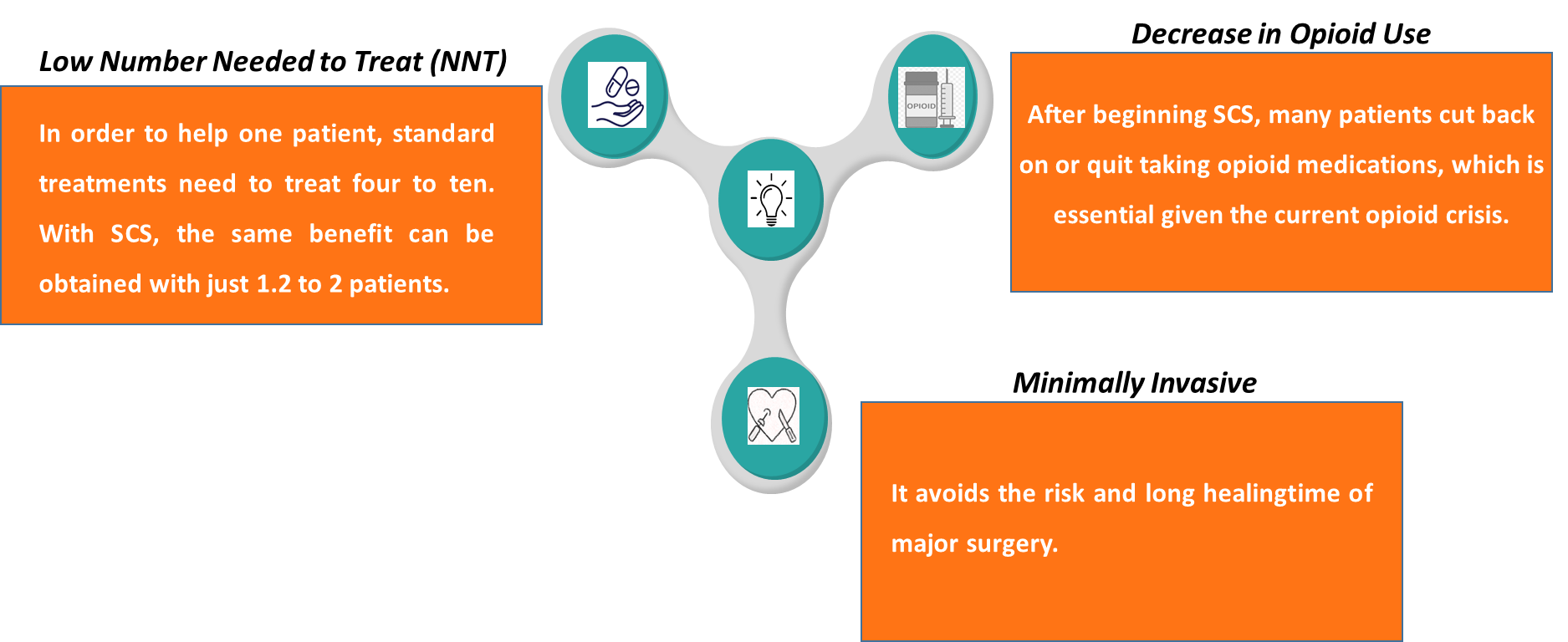
SCS offers consistent, long-lasting results with fewer side effects than drugs or surgery, which frequently only provide temporary or insufficient relief. Important advantages include: [14]
4.3.3 Method of operation
- Trial stimulation: It is essential to determine if the procedure will be successful. The insertion of trial leads is performed under light sedation.
- Permanent Stimulation: During the trial stimulation, data is collected for the number of electrodes required [24].
4.3.4 Evidence-Based Reviews of Spinal Cord Stimulation Treatments for Chronic Pain
Efficacy: Studies have shown that SCS can provide long-term pain relief for up to 50-70% of patients who fail to respond to conventional treatments, and is also associated with improvements in quality of life and reductions in the need for opioid pain medications [12] [14].
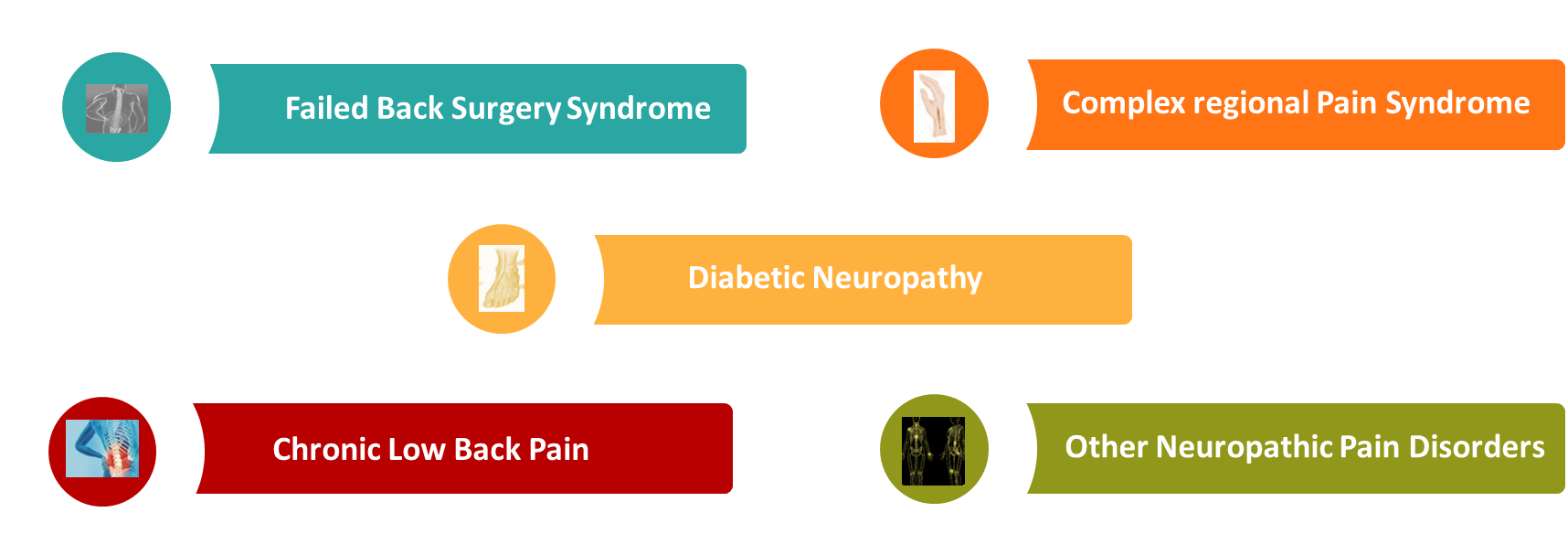
4.3.5 Clinical Application of SCS:
SCS is particularly effective for stubborn nerve pain including: [List would go here if provided]
5. Benefits of Neuromodulation:
Neuromodulation provides a wide range of benefits for patients suffering from chronic pain, especially when other treatments have risks. Here are some of the key benefits [12] [20] [21]:
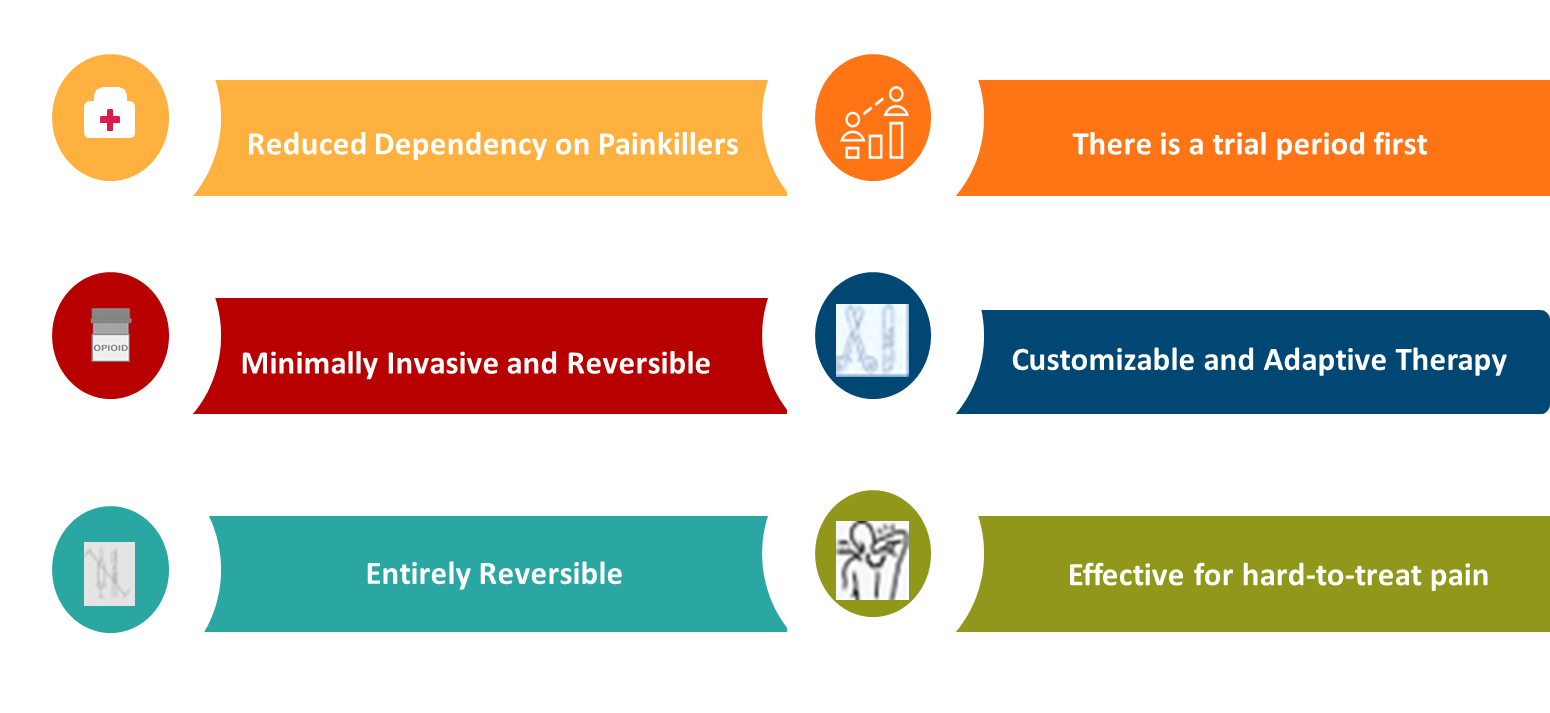
- Reduced Dependency on Painkillers: Addiction is one of the major risks associated with opioid-based painkillers. According to studies, up to 19% of opioid prescription recipients may experience a use disorder. By directly addressing the cause of pain, neuromodulation can drastically cut down on or even completely eliminate the need for these drugs.
- Trial Period First: A temporary trial is performed for one week before the implantation of a permanent spinal cord or dorsal root ganglion stimulator. Temporary wires are implanted into the epidural space with an external battery pack for stimulation purposes to assess whether neuromodulation is effective for pain relief.
- Minimally Invasive and Reversible: Spinal cord stimulation (SCS) and peripheral nerve stimulation (PNS) offer a benefit over major surgeries. Devices can be implanted during an outpatient procedure, and if a patient doesn't respond to these therapies, the implantable devices can be removed or adjusted.
- Customizable and Adaptive Therapy: Modern neuromodulation devices are customizable. Doctors can adjust the intensity, frequency, and location of electrical stimulation based on pain levels and the patient's response. This provides personalized and adaptable treatment.
- Entirely Reversible: Neuromodulation treatment is completely reversible. If it feels ineffective or is no longer needed, the battery pack and electrodes are simply removed.
- Effective for Hard-to-Treat Pain: It is very effective for conditions that are difficult to deal with, including Failed Back Surgery Syndrome (FBSS) and other forms of neuropathic pain. Clinical studies indicate that it is a safe and effective option when other treatments fail.
6. Future outlook:
Neuromodulation therapy is advancing quickly in the management of chronic pain by modulating nerve activity. Its future is promising as technologies and methods improve. New stimulation techniques, such as burst, closed-loop, and high-frequency stimulation, have expanded treatment options and helped patients feel better.
Technological advances like adaptive closed-loop systems and remote monitoring have made pain control easier and more effective for patients. These advances have increased patient satisfaction and reduced the burden on caregivers. In the future, the integration of AI with cloud computing could make devices more personal and smart, adjusting themselves according to a person’s pain patterns and even predicting pain before it starts.
While neuromodulation may require a large initial investment, it becomes more cost-effective over time and will be increasingly supported by growing insurance coverage. A successful future depends on high-quality, placebo-controlled studies and the use of predictive markers—such as psychological, genetic, and neuroimaging tools—to better select patients who will likely derive the highest benefit.
With ongoing innovation in personalized technologies and a deeper understanding of neurophysiological mechanisms, neuromodulation has all the features necessary to become a centerpiece in chronic pain management, offering more efficient, individualized, and long-lasting relief options.
7. Conclusion:
Managing chronic pain is changing quickly. New, safer, and more effective treatments are emerging that do not rely solely on opioids. Opioids have severe side effects and pose a high risk of addiction. One of the most promising fields is neuromodulation, which uses electrical and magnetic stimulation to alter the way nerves process pain. Techniques like spinal cord stimulation, dorsal root ganglion stimulation, and peripheral nerve stimulation all hold the promise of long-term relief without creating side effects or addiction. Growing technical advances bring much individualization and flexibility in designing systems that better address the patient's specific needs. In the future, technologies such as artificial intelligence, improved methods to determine appropriate patients using biomarkers, and greater insurance coverage may make neuromodulation a standard component of pain management. Moving beyond traditional medications is necessary to address the multifaceted problems of chronic pain, enhance quality of life, and decrease the societal cost of opioid abuse.